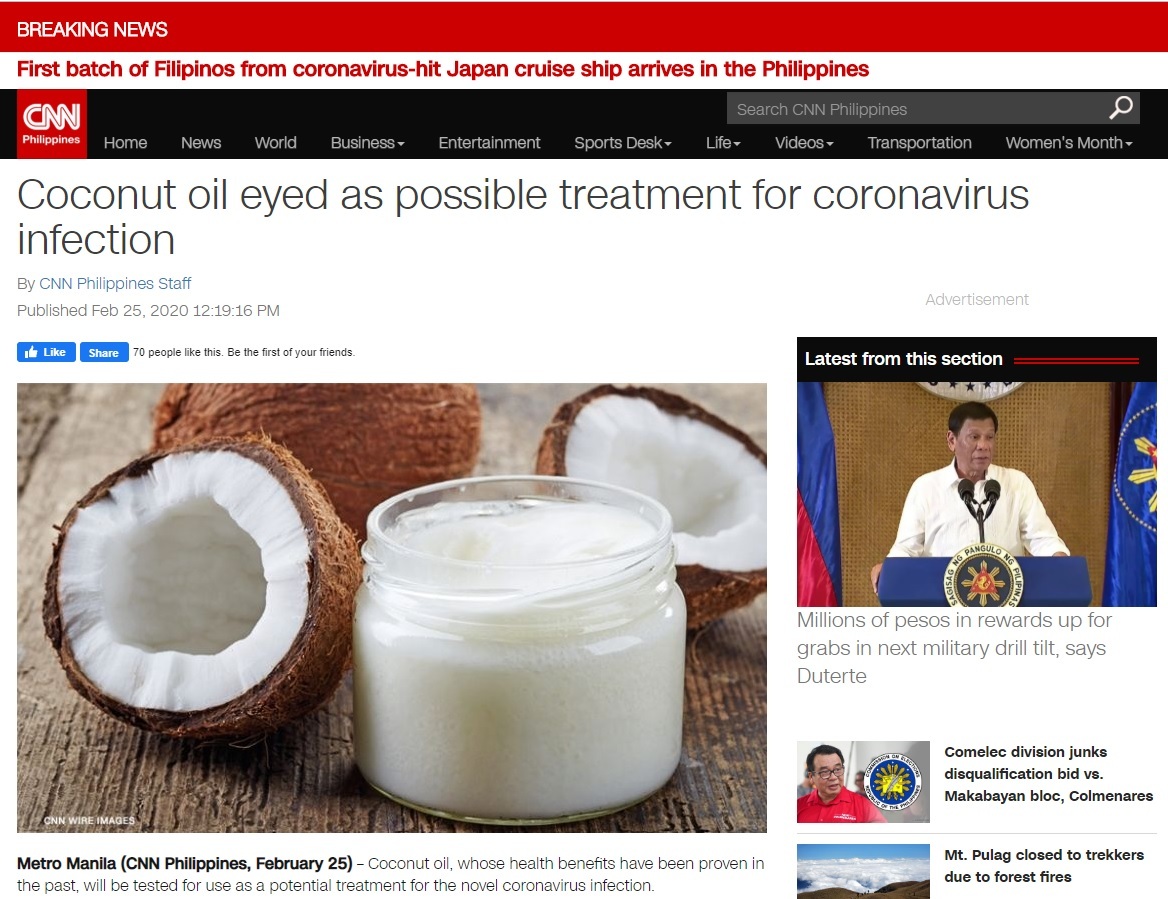
Philippines and Singapore Testing Coconut Oil as Possible Treatment for Coronavirus
Coconut oil, whose health benefits have been proven in the past, will be tested for use as a potential treatment for the novel coronavirus infection. “That [VCO] is being looked into,” Philippine Health Secretary Francisco Duque III told CNN Philippines’ Newsroom on Tuesday. “We have heard very good studies with regard to its ability to neutralize the viruses, but for the COVID- 19, it is not clear,” the top health official added. He made the reaction following Cabinet Secretary Karlo Nograles' announcement Monday that a former academician from one of the country’s top universities proposed to test coconut oil as COVID-19 treatment amid the absence of a specific treatment. In a research proposal published on January 31, Ateneo de Manila University Professor Emeritus Fabian Antonio Dayrit and Dr. Mary Newport of Spring Hill Neonatolody in Florida, United States proposed to conduct a clinical study on patients infected with the COVID-19 involving VCO, saying “this treatment is affordable and virtually risk-free, and the potential benefits are enormous.” Nograles said the National University of Singapore has agreed to test VCO as a prophylactic against the COVID-19. Current evidence suggests coconut oil and its derivatives are safe and effective antiviral compounds in both humans and animals, the researchers noted. “Several in vitro, animal, and human studies support the potential of coconut oil, lauric acid and its derivatives as effective and safe agents against a virus like nCoV-2019 [COVID-19],” they said.