Why The Cholesterol-Heart Disease Theory Is Wrong
by MALCOLM KENDRICK, MD
Redflagsweekly.com
Cholesterol is a much maligned substance, the ‘cause’ of heart disease. If it is, it must have killed billions of people. Far more than the plague, every war ever fought, and all plane, train and car crashes ever – all added together, then multiplied by three.
But if it does cause heart disease, how does it do it? The simple ‘answer’ is that, if you eat too much cholesterol, the level in your blood rises, the cholesterol then travels through the artery wall causing cholesterol-laden plaques to develop which then rupture and kill you. That’s the initial cholesterol hypothesis. Dead simple, couldn’t be more simple.
First little problem – dietary intake of cholesterol has no impact on the level of cholesterol in your blood. If we look at two major long-term studies, Framingham and Tecumseh, it is clear that those who ate the most cholesterol had exactly the same level of cholesterol in their blood as those who ate the least cholesterol.
|
Table: Cholesterol intake – The Framingham Heart Study |
|||
|
Blood Cholesterol |
|||
|
Average Cholesterol Intake |
Below Average Intake |
Above Average |
|
|
mg/day |
mmol/l |
mmol/l |
|
| Men |
704 ± 220.9 |
6.16 |
6.16 |
| Women |
492 ± 170.0 |
6.37 |
6.26 |
|
Table : Cholesterol intake and blood lipids – The Tecumseh Study |
|||
|
Blood Cholesterol in Thirds |
|||
| Daily Intake: |
Lower |
Middle |
Upper |
| Cholesterol (mg) |
554 |
566 |
533 |
This is hardly news. The man, who, more than any other, is responsible for the creation of the diet heart hypothesis fully agrees. To quote Ancel Keys, from a paper in 1956:
‘In the adult man the serum cholesterol level is essentially independent of the cholesterol intake over the whole range of human diets.’
What did Ancel Keys think, more recently, about the connection between cholesterol in the diet, and cholesterol in the blood?
“There’s no connection whatsoever between cholesterol in food and cholesterol in blood. And we’ve known that all along. Cholesterol in the diet doesn’t matter at all unless you happen to be a chicken or a rabbit.” Ancel Keys, Ph.D., professor emeritus at the University of Minnesota 1997.
Does this come as a surprise?
So, it doesn’t matter one jot how much cholesterol you eat, it has no impact whatsoever on blood cholesterol levels. Which just blows up a fairly important part of the cholesterol hypothesis.
‘But, hold on, that doesn’t matter,’ (the sound of goalposts being desperately moved fills the air) ‘It is not cholesterol in the diet that causes the cholesterol level to rise, it is the consumption of saturated fat?’
Look again at the Tecumseh study.
|
Table : Fat intake and blood lipids – The Tecumseh Study |
|||
|
Blood Cholesterol in Thirds |
|||
| Daily Intake: |
Lower |
Middle |
Upper |
| Fat – total (g) |
128 |
134 |
133 |
| Fat Saturated (g) |
52 |
54 |
54 |
| Polyunsat/Sat ratio |
0.51 |
0.51 |
0.51 |
| Cholesterol (mg) |
554 |
566 |
533 |
To explain that table in a little more detail. Basically, it divides people into thirds with high, average or low blood cholesterol levels. The absolute values are not important.
Having done this we can examine the level of saturated fat consumed by these three groups. As can be seen:
- Those in the lowest third of cholesterol levels consumed 52g/day of saturated fat
- Those in the mid-range consumed 54g/day of saturated fat
- Those with the highest levels consumed 54g/day of saturated fat
Which lead to the conclusion, from the authors that:
‘Serum cholesterol and triglyceride values were not positively correlated with selection of dietary constituents.’
I shall translate those weasel words into plain English. ‘You can eat as much saturated fat as you like and it makes no difference whatsoever to your blood cholesterol levels.’
And what of Framingham and saturated fat. Let us quote William Castelli, director of the Framingham study for many years.
| “In Framingham, Massachusetts, the more saturated fat one ate, the more cholesterol one ate, the more calories one ate, the lower people’s serum cholesterol…we found that the people who ate the most cholesterol, ate the most saturated fat, ate the most calories weighed the least and were the most physically active.” Dr William Castelli 1992 (Director of the Framingham study) |
OOOPS!
Now you may think that I am just quoting studies that support my ideas. However, a special prize to the man, or woman, who can find a long-term study showing that a high cholesterol, or high saturated fat diet, has any impact on blood cholesterol levels (in a normal, healthy population). Or, indeed, has any effect whatsoever on the rate of death from CHD.
Quick, time to move those goalposts again.
It’s not saturated fat in the diet, it’s the ratio of polyunsaturated to saturated fat ratio….. the P/S ratio. Hey, can’t you people just give up and admit that fat, of whatever sort, in the diet and cholesterol levels just are not related?
But how could they be? For, in the next episode I shall make it clear that there is no way you can link fat intake with cholesterol levels in the blood. The two substances are completely unrelated chemically, and only ever meet when they are, coincidentally, rammed together inside a lipoprotein.
And then I will show why a high blood cholesterol level cannot cause heart disease. Ladies and gentlemen, roll up, roll up and gasp in amazement as the fearsome cholesterol hypothesis disintegrates in front of your very eyes.
2
Why The Cholesterol-Heart Disease Theory Is Wrong
Part 2
by MALCOLM KENDRICK, MD
Redflagsweekly.com
Some studies have shown that a high saturated fat intake raises cholesterol levels; others have shown the exact opposite. The longest, most prestigious and widely quoted long-term study on CHD, the Framingham study, clearly shows that those who eat the most saturated fat have the lowest cholesterol levels.
My own belief is that in healthy people, dietary intake, of anything, has no effect on cholesterol levels – beyond a few percentage points of non-significant wobble.
But my belief is not an act of personal faith with no foundation on fact. For the science of fat metabolism confirms that there cannot be any connection whatsoever between saturated fat consumption and cholesterol levels. And I am wondering how best to explain this without getting too technical.
The first point to make is that you do not have a cholesterol level in your blood. Cholesterol is insoluble in blood, and therefore has to be carried around the body inside a small sphere known as a lipoprotein. There are many different types of lipoprotein, ranging from the monster chlyomicron to the teeny, weeny, High Density Lipoprotein (HDL).
Lipoproteins do not just carry cholesterol. They also carry all sorts of other fats, saturated, monounsaturated and polyunsaturated. These fats are all attached to a glycerol molecule, in sets of three, and the resulting substance is therefore called a triglyceride.
Triglyceride = three fats attached to a backbone glycerol molecule. (Just in case you’re wondering, a fat is a fatty acid, and a fatty acid is a fat).

Thus, when you eat cholesterol and saturated fat, they are both absorbed into the intenstinal wall, where the saturated fats are all stuck onto a glycerol molecule, to make triglycerides, the cholesterol remains unchanged. Then, within the intestinal wall both are rammed into a chylomicron before being expelled into the portal circulation system to be moved around the body.
Most chylomicrons go directly to the liver where they are absorbed, broken down, and reconstructed into a smaller type of lipoprotein known as a Very Low Density Lipoprotein VLDL. These VLDLs then go out into the general circulation and gradually lose triglyceride. As they do so, they get smaller, transforming from VLDL to Intermediate Density Lipoproteins (IDLs), then Low Density Lipoproteins (LDLs).
The LDL is either absorbed back into the liver, to be reused to create more VLDLs, or they are absorbed into other tissues where the contents are used by the cell.
So, at what point does saturated fat get turned into cholesterol?
Answer, it doesn’t. You don’t make cholesterol out of saturated fat. Cholesterol, when it is made in the liver, starts out as a substance called Acteyl-co A. This is not a fat; it is nothing like a fat. It has several nitrogen atoms in it, and nitrogen comes from protein.
A Saturated Fat* Cholesterol


Point one, therefore, is that saturated fat and cholesterol and copletely unrelated chemically, and you don’t make cholesterol from fats. So why would eating saturated fat increase cholesterol production in the liver?….. It can’t and it doesn’t.
But of course, the substance we are interested in nowadays is LDL. Which is not the same thing as cholesterol at all. So why do we called a raised LDL level a raised cholesterol level?
In fact, the nomenclature in this whole area is just designed to make things almost impossible to understand. For example, a raised VLDL level is known as hypertriglycerideamia. Why? Goodness only knows. Perhaps if researchers in this area were to use a clear form of nomenclature, the weakness of the diet/heart hypothesis would be more easily exposed.
Time for a little review
- Cholesterol and saturated fats are unrelated substances and you don’t make cholesterol from saturated fat, or any other type of fat
- A raised cholesterol level is, in reality, a raised LDL level
- A raised VLDL level is called hypertriglyceridaemia
- The only connection between saturated fats and cholesterol is that, because they are insoluble in water, they sit inside lipoproteins in order that they can be carried around the body
- The liver doesn’t make LDL – LDL is the metabolic residue of VLDL.
Suddenly the whole concept of saturated fat intake raising cholesterol levels doesn’t seem so simple anymore, does it? But, if the substance in the blood that causes CHD is actually LDL, maybe we just need to move the goalposts….again, and ask a different question.
Does a high saturated fat intake increase LDL levels?
Just to review some of the facts. The liver doesn’t make LDL, it makes VLDL, and when VLDL loses triglyceride it turns into LDL.
So, if you eat more saturated fat (or any other kind of fat), the liver will churn our more VLDL. NOT because there is more cholesterol around, but because there are more triglycerides around to deal with.
Therefore, presumably, after all the VLDLs have shrunk in size, there will be more LDLs left. Which means that a high fat consumption could lead to a higher level of LDL, via VLDL metabolism – although we have to abandon the whole cholesterol argument at this point, as cholesterol has nothing whatsoever to do with this process, it just gets carried around as an innocent bystander.
But even if you move the discussion onto LDLs rather than cholesterol, there is a further huge and insurmountable problem here. After a meal VLDL levels go up, as you would expect, but the LDL level remains absolutely constant. Absolutely constant….(and there is no delayed response either).
So, the amount of VLDL in the blood is totally unrelated to the level of LDL in the blood. Despite the fact that you ‘make’ one from the other.
What this proves, beyond any doubt, is that the metabolic system tightly controls the level of LDL in the blood. It doesn’t matter how many VLDLs are converted to LDL, the system takes the excess LDL out of play – instantly. It pulls excess LDLs into the liver where it recycles them.
So, although fat intake can increase VLDL production, it has no effect on the level of LDL. Which means that, not only does saturated fat have no effect on cholesterol production in the liver, it also has no effect on LDL levels. In reality, it has no effect at all. And why should it? If you eat too much protein, your blood protein level doesn’t rise. If you eat too much sugar your ‘fasting’ blood sugar level doesn’t rise. Why should fat or cholesterol be any different?
You will not read this type of information anywhere, but here. However, every single fact I have used has been demonstrated many, many times. These are facts beyond dispute. It’s just that no-one chooses to highlight what all of these facts, when brought together, actually mean.
- Fact one: The liver does not use fats, saturated or otherwise to make cholesterol
- Fact two: The liver does not make LDL, it makes VLDL
- Fact three: VLDL is converted into LDL through triglyceride loss
- Fact four: VLDL levels and LDL levels are totally unrelated – totally
Which means that: Saturated fat intake has no impact on LDL levels.
3
Why The Cholesterol-Heart Disease Theory Is Wrong
Part 3
by MALCOLM KENDRICK, MD
Redflagsweekly.com
SA Raised LDL Level Has No Impact On Heart Disease
Having previously demonstrated that neither cholesterol, nor saturated fat consumption, can have any impact on LDL levels. I now intend to make it clear that a raised LDL level has no impact on heart disease (CHD).
As most of you probably know, current thinking in CHD is that when the level of Low Density Lipoprotein (LDL) is raised, LDLs travel through the artery wall and form a big lumpy cholesterol deposit (‘plaques’) that narrow the arteries. Cholesterol is found in plaques because LDL contains lots of cholesterol.
As these plaques get bigger they narrow the artery so much that blood flow is obstructed – causing symptoms such as angina. Finally a plaque may burst, causing a blood clot to form over the ruptured area. This blocks the artery completely. A myocardial infarction results, which may or may not kill you.
I agree with this basic mechanism underlying CHD, but there are about eight million problems with the idea that a raised LDL is the cause. Let’s just concentrate on three:
1: People with normal and even low LDL levels develop plaques and die of CHD.
Which means that we have a disease process on our hands that can occur when the LDL is level is high, average or low. The first ever example in medical history whereby a normal level of a normal (and vital) substance in the blood can cause a disease.
Yes, LDL is so terrible that any level at all can kill you. The only good LDL is a dead LDL – or words to that effect. This concept, that a normal level of substance in the blood can cause disease, is absolutely nuts and runs contrary to all of biological science, or any other type of science. ‘My goodness you have a NORMAL LDL level, it must be lowered.’
Leaving that aside, for the moment, let’s move to problem number two.
2: LDL can’t get through the lining of the artery wall
The endothelium – single cell lining of the artery wall – is impermeable to LDL – unless you get the level to about three times normal, which is 15mmol/l, rather than 5.0mmol/l. So how does LDL get through in the first place? Considering that 99% of the population has an LDL level below 10.
Answer, you can’t get it through. And even if it could, you run into problem number three:
3: Plaque distribution
Plaques are discreet ‘lesions’ in the artery wall, they are not present everywhere in all artery walls. So, if LDL ‘leaks’ through the arteries when the concentration is raised, then it should leak through all artery walls everywhere, and what we should see, therefore, is thickened artery walls full of LDL everywhere, which is exactly what we don’t see.
To use an analogy, if you lie in the sun for too long, all of your body will become sunburned, not just a few bits here and there. But we are expected to believe that, if you bathe the artery wall in a high level of LDL, it will only leak through in a few discreet areas. Hmmmmm? Again, quite frankly, bonkers.
I know what you are thinking at this point, I think. Aha, you are thinking, obviously you need to damage the artery wall, in discreet areas, to get LDL through…… Exactly. And this could hardly be more obvious. So, the underlying process that starts a plaque is damage to the endothelium. Of course it is; there is no other possible explanation.
But, to admit this, is to admit that LDL has nothing whatsoever to do with causing atherosclerotic plaques, because LDL doesn’t damage the endothelium.
Faced with this major, and I would say insurmountable problem, what has the cholesterol/LDL brotherhood chosen to do? Discard the diet-heart/cholesterol/LDL (whatever it is now called) hypothesis. Or keep trying to find ways to explain the causal role of LDL in plaque formation.
No surprise to find that no-one was remotely willing to discard the hypothesis. This square peg of orthodoxy had to be rammed into the circular hole of CHD causation at all costs. Otherwise the entire diet-heart/cholesterol/LDL hypothesis collapses into a little heap of dust.
So where are we now? How exactly does LDL cause CHD?
Because it is oxidised.
You may faintly detect the sound of me beating my head against a wall in the distance, somewhere just south of Manchester UK.
Because, dear reader, LDL is oxidised! You have probably heard of anti-oxidants, and their magical protection against CHD. But how are they thought to provide this protection? Mainly because oxidised LDL can be absorbed by the endothelium, as there are receptors for oxidised LDL on endothelial cells (called Lox-1 receptors, if you are interested).
So, the thinking goes, once oxidised, the LDL binds to the Lox-I receptor it is then transported into – then through – the endothelium and into the artery wall behind. At which point, white blood cells, designed to get rid of all nasty substances in the body, attack, engulf and try to clear away all of the oxidised LDL molecules.
But these white cells have no means to tell them to stop engulfing oxidised LDL, allegedly, so they just get bigger and bigger until they explode, releasing a horrible goo of dead white blood cells, bits of LDL, cholesterol and triglyerides etc. into the artery wall. Once you have enough exploding white blood cells, the lump of goo becomes big enough to start an atherosclerotic plaque. And that is why oxidised LDL is such a bad thing, and why anti-oxidants are protective.
There are so many problems with this proposed mechanism of action that it is almost impossible to know where to start. Perhaps the best place to start is with a previous example.
If there are receptors for oxidised LDL on endothelial cells, then oxidised LDL will be absorbed through all artery walls everywhere, and therefore we would not see discrete plaques forming, just general thickening of all artery wall as they fill up with the residual goo from exploding white blood cells. But we do see discreet plaques, and therefore? Therefore the hypothesis is wrong as it does not match the observed disease process.
The other problem is just as serious, although a little more difficult to explain.
If plaques are created by oxidised LDL, then the ‘cause’ of CHD must be excess oxidisation of LDL in the bloodstream. If this is true, then the level of LDL is completely irrelevant, it is only the amount of oxidised LDL that counts. Therefore, if you believe in this hypothesis, then the ‘raised LDL causes CHD’ hypothesis has to be discarded.
In essence, you can’t have this argument both ways. You can claim a raised LDL causes CHD – in which case how can people with a low level get CHD? Or you can claim that excess oxidised LDL causes CHD. In which case CHD has nothing to do with LDL levels.
Ironically, the oxidised LDL hypothesis – which was supposed to protect the LDL hypothesis – actually destroys the LDL hypothesis. But by throwing up so much jargon and incomprehensible mechanisms of actions into the air, it appears that you are keeping both hypotheses going. But you can’t, it’s one or the other, you can’t have both.
And by the way, in the Heart Protection Study (HPS), which lasted five years, ten thousand patients received the anti-oxidants and ten thousand patients did not. And the results?
‘’’There was no evidence of any benefit at all’ from antioxidant vitamins. On the other hand, there was no evidence of any harm.’’’ Dr Rory Collins BMJ Nov 2001
So, bang goes the anti-oxidant hypothesis. Please spare me the claim that they used the ‘wrong’ anti-oxidants.
Once again, as with almost every part of the diet-heart/cholesterol hypothesis, when you start to examine the facts objectively, the whole thing starts to disintegrate in front of your very eyes. There is no way that LDL, oxidised or otherwise, can ‘cause’ CHD, and here are a few more facts to back this up.
Framingham first:
There is a direct association between falling cholesterol levels over the first 14 years and mortality over the following 18 years (11% overall and 14% CVD death rate increase per 1 mg/dL per year drop in cholesterol levels). Anderson KM JAMA 1987
In Framingham therefore, as LDL/cholesterol levels fell, CHD rates went up.
Then Honolulu:
‘Our data accord with previous findings of increased mortality in elderly people with low serum cholesterol, and show that long-term persistence of low cholesterol concentration actually increases the risk of death. Thus, the earlier that patients start to have lower cholesterol concentrations, the greater the risk of death.’ Lancet Aug 2001
In Honolulu, the lower the LDL/cholesterol, the greater the risk of dying – of everything, including CHD.
Then Russia:
The main author of the report on this study was Shestov, of the Institute of Experimental Medicine, Russian Academy of Medical Sciences, St. Petersburg. And the main conclusion of this study was as follows:
‘The results disclose a sizeable subset of hypocholesterolemics in this population at increased risk of cardiac death associated with lifestyle characteristics.’ Russian Lipid Research Clinics Prevalence Follow-up Study Shestov
In Russian, a greater risk of death from heart disease in those with low blood LDL/cholesterol levels
Then Japan:
Between 1980 and 1989, age-adjusted total serum cholesterol levels increased from 4.84 to 5.22 for men and from 4.91 to 5.24 mmol/l for women. Prevalence of age-adjusted hypercholesterolaemia of > or = 5.68 mmol/l increased from 15.8% to 29.4% for men and from 18.4% to 30.6% for women…. Considerable increases in total serum cholesterol levels do not offer an explanation of the recent decline in mortality from coronary heart disease in Japan.’ Okayama A, Marmot MG Int J Epidemiol Dec 1993
In Japan, as cholesterol/LDL levels went up, death rates from CHD went down.
How much more evidence would you like? Perhaps another study from the USA?
‘Kummerow and colleagues from the UI and Carle Foundation Hospital in Urbana, Ill., studied 1,200 patients who were cardiac-catheterized. Sixty-three percent had at least 70 percent of their arteries blocked — enough to warrant bypass surgery. Of the 506 men who had a bypass, only 71 (14 percent) had plasma cholesterol levels above 240 (6.2mmol/l); 50 percent had levels below 200 (5.2mmol/l). Thirty-two percent of the 244 women who had bypass surgery had levels above 240 (6.2mmol/l); 34 percent were below 200 (5.2mmol/l)…
… a 3-to-1 ratio of LDL (bad cholesterol) to HDL (good cholesterol) is a low heart-disease risk? with a total cholesterol of less than 200 (5.2mmol/l) being the most desirable. However, in this study, Kummerow noted, 51 percent of the catheterized men had levels below 200 (5.2mmol/l) but needed a bypass.’ Paper by Kummerow Atherosclerosis March 2001
In this study, the majority of men who needed a bypass had cholesterol levels below 5.2mmol/l.
These were not, I will add, small studies, with surrogate end-points. These were great big studies done on thousands and thousands of people, and they measured death rates and blockages in coronary arteries, which are ‘hard’ end-points. They include Framingham – the study that is used to set the CHD prevention guidelines! And they all demonstrate very clearly that the rate of CHD has nothing whatever to do with the level of LDL/cholesterol in your bloodstream.
These studies were also published in journals as prestigious as the Lancet, Atherosclerosis and JAMA. This is not wacky, fringe research, carried out by people with a distrust of mainstream medicine. This is as mainstream and conventional as it gets, and all of this research utterly and completely contradicts the current cholesterol/LDL theory of CHD. And I will bet that you have never, ever, come across these facts before. For some strange reasons this research doesn’t get a lot of publicity.
Ah but, you might say, statins reduce LDL levels and protect against CHD. Surely that proves – despite your clever arguments, and all of the evidence – that a raised LDL truly is the cause of CHD, even if it is biologically impossible.
Well, for those of you who are interested, I can easily prove that the LDL lowering effects of statins have nothing whatsoever to do with their impact on CHD.
4
Why The Cholesterol-Heart Disease Theory Is Wrong
Part 4
by MALCOLM KENDRICK, MD
Redflagsweekly.com
Statins reduce the risk of dying of coronary heart disease (CHD). There, I said it. You probably thought I didn’t believe this, but you can’t argue with the results from the clinical trials. Big, long, well-controlled studies that have all shown pretty much the same thing – stains provide protection against CHD.
Should this be a surprise? Statins were, after all, specifically designed to block the synthesis of cholesterol in the liver, and thus reduce LDL/cholesterol levels in the blood – and they do this very well. Furthermore, by reducing the level of LDL, statins were then supposed to reduce the risk of CHD – on the basis that a raised LDL level was the primary risk factor for the disease – and they do this too.
On the face of it, a glorious vindication of the ‘cholesterol hypothesis’ of CHD, and it looks pretty damned inarguable doesn’t it? Raised LDL levels cause CHD, and when they are lowered, the risk of CHD drops. Cause and effect flushed out into the open. Experimental proof. Touché.
So, Batman, argue your way out of that!
Let us start the argument with a little diversion into the world of risk. You may have seen figures stated, such as, ‘statins reduce the risk of CHD by 40%, even 50%.’ You may not know what such figures mean. They certainly sound super-impressive, and suggest that a statin will save one person’s life for every two people taking the drug. Right?
Wrong.
For that risk reduction is a relative risk reduction – not an absolute risk reduction. To explain.
The risk of being struck by lightening (I’m guessing here), may be one in five million over five years. Were I to develop a hat with a copper wire reaching from it down to the ground, the amazing copper-o-matic, I may reduce your risk of a lightening strike over five years to one in ten million, an amazing 50% reduction in risk.
The other way to look at this is that your absolute risk of being struck by lightening has changed from 0.000.02% to 0.000.01%. Or an absolute risk reduction of 0.000.01%. Take you pick, a massive 50%, yes 50% risk reduction. Or a measly 0.000.01% risk reduction.
They both mean exactly the same thing, but one sounds a bit more impressive than the other, and were I to try to sell you my copper-o-matic – $19.95 from all major stores – I know which type of risk reduction I would be promoting (And no, it wouldn’t be absolute risk reduction)
Thus, if we look at the recent Heart Protection Study, hailed as the most amazing trial ever, at least by the chief investigator anyway, this showed that tens of thousands of lives could be saved each year by the use of statins, with a risk reduction of nearly 50%.
True, all true, but how many people would you need to treat to save fifty thousand lives?
The figures from the HPS were that you could save fifty thousand lives, over a five year period, if you treated….. Have a guess.
Ten million people.
This works out at one life saved for every two hundred people treated, or an absolute risk reduction of 0.5%. Maybe not quite as awe inspiring as you may have thought. About the same risk reduction, in fact, as is achieved by aspirin.
And, if we take these figures a little further, it is possible to work out something else quite interesting, which is that a lifetime reduction of LDL using statins will result in a, maximum, 3% risk reduction of dying from CHD.
To explain. If a statin reduces the risk of dying of CHD by 0.5% over five years, and you take a statin for thirty years, basically a lifetime of drug taking, then you would have a 0.5% x 6 reduction in risk. Or 3%. Which opens up an interesting thought. Interesting to me, at least.
In general, statins bring LDL levels down to the ‘normal’ level, but by doing so they decrease your risk of dying of CHD by a somewhat titchy 3%. Which, even if you do believe that statins work by lowering LDL levels, leaves a rather large 97% of CHD caused by something else, other than a raised LDL level – and what might that be?
Anyway, to return to the main point, which is that, whilst statins do ‘normalise’ LDL levels, they don’t actually provide that much protection against CHD. Which means that it could well be that their ‘protective’ effects may be due to something else, other than LDL lowering. (On the other hand, if the absolute risk reduction was 50%, then I think this would be case proven for the cholesterol hypothesis).
Even so, I recognise that to suggest that the cardioprotective effects of statins are, in effect, a coincidence, seems a bit of a stretch. But bear with me, for I think that case for coincidence is overpoweringly strong.
There are four main strands to the coincidence argument:
- Statins act far too quickly for it to be through any LDL lowering effect
- They work independently of the LDL level – or by how much they lower the LDL
- Statins protect against CHD in the elderly, in whom a raised LDL level is not a risk factor
- They have many other effects, other than lowering LDL levels, a great number of which have been clearly demonstrated to have an beneficial impact on both blood clotting and endothelial damage – and thus CHD
Speed of action
It is generally accepted that a raised LDL level takes many years to cause CHD. Exactly how many is unclear, but the major clinical trials on statins lasted five years, so the assumption here was that it would take at least five years on a statin to show any significant effect on the rate of CHD.
If, however, statins reduce CHD risk within a much shorter time period, this makes it almost certain that they are not working through LDL lowering.
So what of the: Myocardial Ischaemia Reduction with Aggressive Cholesterol Lowering (MIRACL) trial on the short term use of statins?
‘MIRACL demonstrated that intensive treatment with atorvastatin, begun immediately after an acute coronary event, produces beneficial effects that are apparent within several weeks. This provides evidence that the addition of intensive lipid-lowering therapy to the standard of care may help improve the outcomes of these patients.’ – Dr Gregory Schwartz.
Statins work within weeks, not months or years. Actually, to have a measurable effect within weeks, they must be working immediately – instantly. Because If they didn’t start working for weeks, they wouldn’t show any effect for months. And this is not a one off result; it has been shown in many trials.
‘Lipid-lowering therapy after acute coronary syndromes (ACS) reduces risk of 6-month mortality by one third after adjustment for confounding factors and should be prescribed to patients in order to reduce short-term mortality.’ – Dr Herbert Aronow Lancet Apr 2001
On thing is absolutely certain, these short term protective effects cannot be due to LDL lowering.
Dose response
Moving on to the next point. If statins do work by lowering LDL, then the more that LDL is lowered, the more CHD protection you should see. In fact, a number of trials have shown the exact opposite:
‘…(in the CARE trial) In addition, there was no linear relationship between the extent of LDL reduction and percent reduction of events. Patients whose LDL levels on treatment were between 101mg/dl and 125mg/dl had a 46% event reduction, while those treated below 100mg/dl only enjoyed a 32% event rate reduction. – Thomas Bersot MD. AHA 71st Scientific Sessions Nov 8 – 11 1998
And if you look at other trials on statins, you cannot see any dose response, just a general reduction in CV events with statins, no matter what the starting level of LDL or how much it is lowered by.
Effect in the elderly
As demonstrated in earlier articles, there is no doubt that a low cholesterol/LDL level is associated with higher rates of CHD in the elderly. Yet, if you give statins to elderly patients they are protected against CHD. In addition, in the recent Heart Protection Study, statins also protected against Ischaemic stroke, and a raised LDL level is not a risk factor for this condition.
So statins work immediately, they work independently of their LDL lowering effect, and they work in populations, and conditions, where a raised LDL is not a risk factor. All of which makes it inarguable that their CHD protecting effects have nothing to do with LDL lowering. They must operate in another way.
Other effects
When statins first came out and started to show protection against CHD, I must admit that my conviction that LDL levels have nothing to do with CHD was severely shaken. Indeed, for a few years I gave up on my alternative hypothesis.
However, it didn’t take too long for data to start emerging that cast serious doubts over the ‘statins protect against CHD by lowering LDL levels’ concept. I wasn’t the only one to notice the difficulties with the data:
The statins correct plasma lipid levels optimally, yet the real magnitude of their benefits is marginal and certainly not better than attained with agents that do not affect plasma lipid levels. It is suggested that some of our recommendations and actions relating to plasma cholesterol levels and to atherosclerosis are based on concepts that are fundamentally flawed and need to be revised. – Krut LH Am J Cardiol 1998
So what else were statins doing?
The beneficial effects of statins on clinical events may involve nonlipid mechanisms that modify endothelial function, inflammatory responses, plaque stability, and thrombus formation…These nonlipid properties of statins may help to explain the early and significant cardiovascular event reduction reported in several clinical trials of statin therapy. – Rosenson RS JAMA 1998
In reality, statins do all sorts of things that could easily provide protection against CHD, dividing into three basic areas:
- Plaque stabilisation
- Endothelial protection
- Anti-coagulation
As you may be aware, the latest hot thing in CHD research is to measure C – reactive protein levels (CRP). The CRP level provides a reasonable indication of endothelial ‘damage,’ with higher levels suggesting active plaque formation and growth. So if statins work by reducing endothelial damage, rather than by lowering LDL, we should see statins lowering CRP levels. And guess what….statins reduce CRP levels.
It will not be too long (in fact it is happening now) before mainstream researchers start to actively promote the fact that statins protect against CHD by protecting the endothelium, and thus lowering CRP. In time the LDL lowering effects will, like the Cheshire cat, gradually disappear until you will never know they were there at all.
At which point the entire diet-heart/cholesterol LDL hypothesis should just roll over quietly and die, killed, ironically, by the statin data. But this hypothesis has proven before that the small matter of several mortal wounds has no effect upon it. The inescapable fact that statins do not, and cannot, work by lowering LDL levels will, I predict, prove merely an inconvenience.
For the cholesterol hypothesis managed to survive the fact that cholesterol in the diet has no effect on cholesterol levels in the blood – by claiming that it was saturated fat that mattered all along. It easily shrugged off the data showing that many people with ‘normal’ cholesterol levels died of CHD – mainly by lowering the definition of normal. I think it has now reached 4.5mmol/l, but it has a few more mmol/l to fall yet.
So the statin data will be blithely ignored. The diet-heart hypothesis will simply change its shape and grow again, stronger than before. It is the original 1950s B-movie monster hypothesis.
5
Why The Cholesterol-Heart Disease Theory Is Wrong
Part 5
by MALCOLM KENDRICK, MD
Redflagsweekly.com
Women don’t’ suffer as much CHD as men – of the same age – despite having slightly higher LDL levels. I’m talking here about women under the age of about seventy. After that the statistics become horribly inaccurate and, in the end, we all have to die of something.
For years and years it was suggested that women were protected against LDL by their sex hormones. In fact the ‘sex hormones protect women against CHD’ hypothesis became an accepted fact, a given.
Like most people, I accepted it too, in “a kind of, I can’t be bothered checking out every fact that I hear,” sort of a way. Anyway, superficially, it made sense. Women have similar risk factors (usually higher LDL levels), they suffer about one third the rate of CHD, and they have hormones. Ergo, it is the hormones that protect women. Nice and simple: To quote H.L. Mencken on simple solutions.
‘For every complicated problem there is a solution that is simple, direct, understandable, and wrong.’
However, as with almost every other known ‘fact’ about CHD, if you do choose to look for the evidence, it doesn’t exist. For years I assumed that someone had carried out a massive pivotal trial proving that female sex hormones really were protective. But when I went to look for it, I found that the cupboard was bare. This fact, quoted endlessly, with utter conviction, is based on absolutely nothing at all.
It is true that oestrogen and progesterone (as we call them in the UK), have some beneficial impact on lipids and blood coagulability, but in fact, if you look hard enough you can find effects on almost everything in the cardiovascular system. Any of these effects could, theoretically, have some protective benefit. And lo it was decided that these ’test-tube’ benefits really were important.
Perhaps the most important of these effects was an increase in High Density Lipoproteins (HDLs), otherwise known as ‘Good Cholesterol.’ I love the idea of good and bad cholesterol; it’s like something out of Star Wars. ‘This cholesterol has gone over to the dark side…”
Give us a break ‘Good’ and ‘Bad’ cholesterol. How scientific is that? And HDL isn’t cholesterol anyway. It’s a lipoprotein. But the very fact that such emotive words as good and bad have slipped into this area is a powerful indication that the cholesterol/diet-heart hypothesis is not driven by reason, but by emotion. Frankly, that is the only reason why a hypothesis that makes absolutely no sense whatsoever has survived this long.
Anyway, to return to sex hormones, HDL, and female protection against heart disease. It is true that a high HDL level is associated with a lower rate of CHD. I don’t think that anyone could argue with this, not even me, and I can pick a fight in an empty room. For this reason, it was decided that HDL protects against CHD. Quite how, is lost in the mists of time.
Again, it is true that HDL ‘picks-up’ loose cholesterol from dead cells and transports it back to the liver, using the ‘reverse cholesterol transport system.’ But if you want to explain how it manages to suck cholesterol out of an atherosclerotic plaque, then you are going to have to travel well past the realms of the improbable, and into the zone of the completely impossible.
HDL is travelling through an artery when, suddenly, it spots a cholesterol laden plaque. It stops at that exact point and transports itself through the endothelium. Bravely, battling against a concentration gradient, our plucky HDL locks onto the plaque, sucks cholesterol out, changes direction, reverses back through the endothelium and into the bloodstream. From there to the liver where it heroically unloads its package of ‘Bad cholesterol.’ File under: Great Myths of the Western World.
Despite this, it has become another established truth that HDL is not just associated with a reduced rate of CHD; it is, in fact, an active protective factor. Oh, would someone please set up a university dedicated to teaching the difference between an association, a cause, and an effect. All researchers into CHD will be forced to attend, and beaten with large clubs until they finally understand that when you find factor X is raised in condition Y, it does not mean that factor X causes condition Y. Other explanations are possible – thwack! ‘Repeat after me, other explanations are possible.’ Thwack! ‘And have another Thwack for good measure – you dolt.’
From this, you may be able to gather that I am not a great supporter of the hypothesis that HDL protects against CHD. So it came as no great surprise to me to find that, although HRT raises HDL levels and thus, according to accepted wisdom, should protect against CHD, when this was finally studied, guess what?
The rate of CHD in women on HRT went up. Despite the increase in HDL, (and a decrease in LDL). To quote from the conclusion of the heart and estrogen/progestin study.
Conclusion
‘Although many mechanistic and observational studies suggest that estrogen or estrogen plus progestin reduces the risk of morbidity and mortality from CHD in postmenopausal women, the HERS (The heart and estrogen/progestin study), the only large, randomised, controlled study of this question to date, failed to confirm this. Until data from ongoing studies are available, health care providers must reconsider prescribing ERT or HRT for the secondary prevention of CHD.’
This study was completely negative. Actually it was worse than negative; death rates from CHD rose in the first year of treatment. And these results were confirmed by a further study called ‘The effects of estrogen replacement on the progression of coronary-artery atherosclerosis.’ This too showed no benefit of HRT on CHD. These results have been so negative that the American Heart Association was forced to re-write their guidelines in 2001, and now recommends strongly against using HRT to protect against CHD.
Not only, it would appear, do female sex hormones fail to protect against CHD. They actually make it worse.
In reality, what has happened with women, and CHD, is something that I consider to be quite extraordinary. Over the years it gradually became a ‘known fact’ that a high cholesterol/LDL level causes CHD, yet it was also discovered that women had high cholesterol levels and low rates of CHD, so an ad-hoc hypothesis was developed, which is that women are protected by their sex hormones. This in itself is not extraordinary; it’s what happened next.
And what happened is that the sex hormone theory became so popular that it, in turn, become a ‘known fact,’ despite a complete and utter lack of evidence. In fact, whenever anyone has studied female sex hormones in relation to CHD they have only found results that completely contradict the ‘protection’ hypothesis. Yet, this is just completely ignored. Swept blithely under the carpet.
When I have discussed this issue with researchers in the area they merely shrug and state words to the effect, ‘Oh well, they must be protected by something else then.’ No attempt to state what the amazing protective ‘factor’ may be? But, of course, we are now into the ‘Neptune is angry’ form of circular argument.
‘Why do women, who have LDL/cholesterol levels just as high as men, if not higher, have a low rate of CHD?’
‘Because they are protected.’
‘How do you know that?’
‘Because they have high LDL/cholesterol levels and a low rate of CHD, and a high LDL/cholesterol level is the cause of CHD, so they must be protected.’
Strip away all of the scientific jargon and this is all that is left of the cholesterol hypothesis when you look at women and CHD. In reality, the rate of CHD in women should be another fatal wound in the cholesterol hypothesis. But, as I have pointed out before, fatal wounds have no effect on the cholesterol hypothesis, or the LDL hypothesis, or the diet-heart hypothesis, or the Omega 3 fatty acid hypothesis – or whatever it has currently mutated into. For this hypothesis is now an article of faith, and you can’t kill faith with facts. For faith, to quote from the Bible:
‘Faith is the substance of things hoped for; the evidence of things not seen.’
Just try arguing against that.



 Studies Continue to Show Coconut Oil Improves the Lives of People with Parkinson's Disease
Studies Continue to Show Coconut Oil Improves the Lives of People with Parkinson's Disease More Studies Prove that Coconut Oil is Best for Oral Health Beating Commercial Products and Drugs
More Studies Prove that Coconut Oil is Best for Oral Health Beating Commercial Products and Drugs HHS Secretary Kennedy Breaks His Promise: "War on Saturated Fat" Kept in Tact with New U.S. Dietary Guidelines
HHS Secretary Kennedy Breaks His Promise: "War on Saturated Fat" Kept in Tact with New U.S. Dietary Guidelines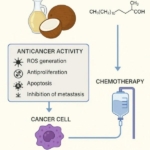 Research Continues to Show Virgin Coconut Oil's Effectiveness in Treating Cancer
Research Continues to Show Virgin Coconut Oil's Effectiveness in Treating Cancer Coconut Oil Continues to Benefit Alzheimer's Patients over Drugs as Studies Continue for Neurological Benefits
Coconut Oil Continues to Benefit Alzheimer's Patients over Drugs as Studies Continue for Neurological Benefits